Get SMART About Compression
With nearly 60% of all cases occurring within 90 days of hospitalization, Venous Thromboembolism (VTE) is one of the leading causes of avoidable hospital death, even though, 7 out of 10 cases can be prevented1. Join us in the fight against Hospital-Acquired VTE — together we can keep patients safe and reduce HA-VTE.
1VTE infographic (lit # 19-134-F)
Featured products
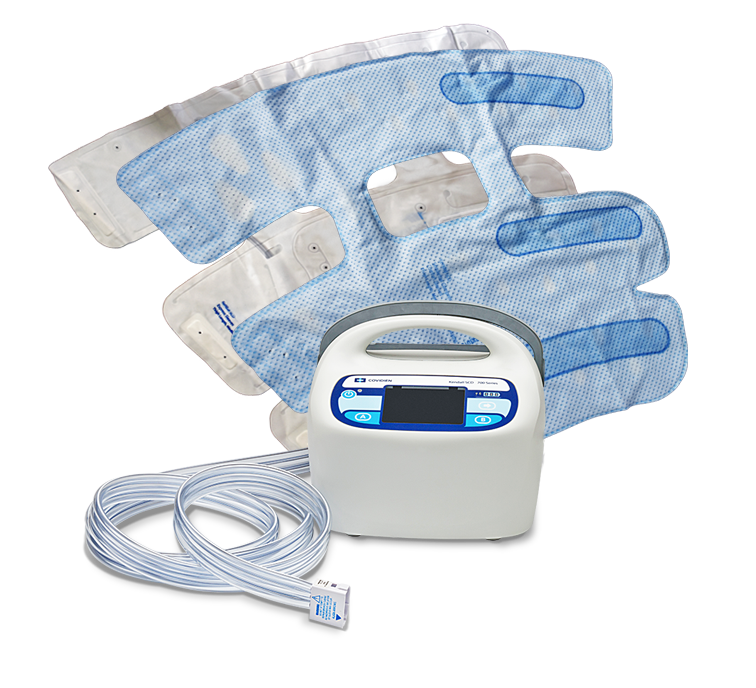
SMART COMPRESSION™ System
The SMART COMPRESSION™ System includes the Kendall SCD™ 700 Series Controller, Kendall SCD™ Comfort and Express Sleeves, and Kendall SCD™ Foot Cuffs. They apply intermittent pneumatic compression to increase venous blood flow, helping prevent deep vein thrombosis and pulmonary embolism in at-risk patients.
T.E.D.™ Anti-Embolism Stockings
T.E.D.™ Anti-Embolism Stockings are clinically proven to reduce the incidence of DVT up to 50%1 and to promote increased blood flow velocity in the legs 138%2 of baseline by compression of the deep venous system.
1Ishak, M.A. and Morley, K.D. Deep venous thrombosis after total hip arthroplasty: a prospective controlled study to determine the prophylactic effect of graded pressure stockings Br. J. Surg 1981; 68: 429-432.
2Sigel B., et al. Type of Compression for Reducing Venous Stasis. Archives of Surgery. 1975; 110: 171-175

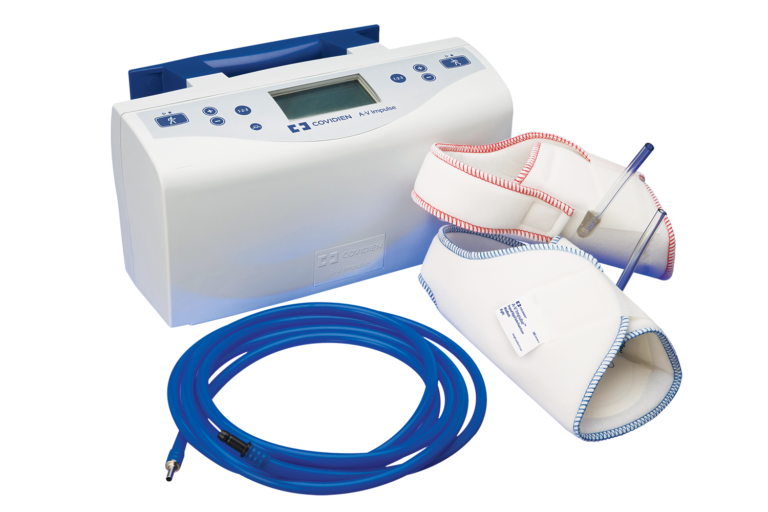
The A-V Impulse™ Foot Compression System
The A-V Impulse™ Foot Compression System mimics the hemodynamic effect of ambulation by flattening the plantar plexus and completely evacuating blood from the bottom of the foot.
Watch the World Thrombosis Day Webinar
Shop all Compression products
Resources
A-V Impulse Brochure



